By: Alice de Souza, Héctor Villa León, Jhoandry Suárez y Zoila Antonio Benito
PUBLISHED: 11-jul-2022
There was no time. Saionara Santana had to rush to get her daughter treated at a medical center in Salvador, the capital of Bahia, in eastern Brazil. The child had chronic colic. When she arrived, her heart in her throat, the receptionist barely looked at her. The situation was urgent so Saionara said the words that she believed would win the receptionist’s understanding.
“I have lupus and I need my daughter to be taken care of,” said the 45-year-old mother.
“Yes? So what?” was the answer she received.

Saionara Santana.- Brazil
In that instant, which lingers as a vivid memory from three years ago, Saionara understood that for the health care system of her country she was just another data point in the Systemic Lupus Erythematosus (SLE) statistics, that pledges of priority because she is a woman, a lupus patient and Afro-Brazilian were nothing more than empty promises. She knew then that a cold and indifferent look would always await her.
What she did not imagine was that her situation was similar to that of other women in the region, especially in Colombia and Peru, where women of African descent face delays in their diagnosis due to slow examinations or a lack of specialists. This gap in the health care system paves the way for lupus to get worse and compromise vital organs, particularly kidneys, according to the article "Global Epidemiology of Systemic Lupus Erythematosus" published in Nature Reviews Rheumatology.
Statistics from the Brazilian Health System (SUS) underscore the gravity of the problem. Some 87% of patients who died between 2016 and 2020 from diseases linked to lupus were women. Of the deaths in those same years, 47% were Black women.
Research published in 2017 in the Brazilian Journal of Rheumatology estimates there are between 150,000 and 300,000 patients with the disease in Brazil.
In Colombia, the number of lupus cases reported by doctors has been steadily rising, from 23,777 in 2015 to 52,944 in 2021.

Mireya Cuesta.- Colombia
In Peru, 16,000 cases were reported in 2020, but researchers believe the number could be higher since many doctors still do not correctly diagnose symptoms as lupus.
Lupus is an autoimmune disease, which means that the immune system – the body system that usually fights infections – attacks healthy tissue instead. It can cause pain and inflammation in any part of the body and is capable of causing organ damage that can leave the patient incapacitated.
Because lupus is such a complex disease, patients are often misdiagnosed. Dr. Santiago Bernal, a rheumatologist and professor at the Universidad Javeriana in Colombia, explains that “one can find a whole spectrum (of symptoms), from patients whose brain is affected, to others whose heart, lungs, kidneys, pancreas, liver, intestine or skin” are impacted.
For Dr. Oswaldo Castañeda, a Peruvian rheumatologist with almost 40 years of experience treating patients with the disease, "it is still very difficult to diagnose [lupus], due to lack of knowledge and acuity.”
Legislative measures have been passed in some Latin American countries to respond to the special medical needs of patients with lupus.
In Peru, Regulations of Law No. 29698 declares the treatment of people suffering from rare or orphan diseases to be of national concern and preferential attention. But in Colombia, the Rare Diseases Law 1.392 which guarantees access to treatment of many rare diseases excludes lupus.

Gumelín Ruíz.- Perú
Discrimination and lack of access to medical services have prevented women of color in countries such as Peru, Colombia and Brazil from getting the medical care they need.
In this special report, women in Brazil, in Peru and in Colombia tell their stories of discrimination, exclusion from the health care system and lack of care. In sharing their experiences, they give voice to the many women of color in Latin America who face inadequate and inequitable treatment for debilitating conditions caused by lupus.
This is the story of Saionara, who has been suffering from lupus since 2018. It’s the story of Jenny Saavedra, a mestizo and Afro-American woman from northern Peru who suffered a psychotic crisis. On the Colombian coast, it’s the story of Mireya, who suffers from episodes of schizophrenia and has kidney and lung damage as a result of the disease.
The Covid-19 pandemic caused a global shortage of hydroxychloroquine, an antimalarial medication that is vital in the treatment of lupus.
During the pandemic, the U.S. Federal Drug Administration gave doctors emergency use authorization to treat Covid patients with hydroxychloroquine and then revoked the authorization after some of the patients suffered serious heart rhythm problems and other medical issues such as blood and lymph system disorders, kidney injuries and liver problems and failure.
But with the world’s attention on hydroxychloroquine as a possible treatment for Covid, the medication was suddenly in short supply.
In Colombia, Camila Castellanos, 25, went up to 20 days without receiving the hydroxychloroquine because of its massive use to combat the coronavirus.
"You can't go without this medicine. Demand it," her rheumatologist told her, so she even threatened her Service Provider Entity (EPS), the equivalent of health insurance, with legal action if they did not give her a solution.
"I was very scared and was only thinking that lupus doesn't wait; I felt at risk," Camila says. She finally managed to be transferred to another institution where she was given hydroxychloroquine.
The hydroxychloroquine shortage was evident in Peru and Brazil as well, and led to the creation of support networks among SLE patients to seek medication that was in scarce supply or to obtain donations.
In Brazil, prescriptions were required in order to buy hydroxychloroquine at pharmacies. "The problem was that no one could talk to their doctors to get the prescription. Now things are back to normal, but those who live far from the capitals still suffer from the lack of access," said Eduardo Tenório, president of the NGO Superando o Lúpus.
"The box doubled in price; it was very complicated for me. Now that I am back in my city and without a job, separated, I depend on my mother's money to buy the next boxes," said Irma de Almeida, the lupus patient in Roraima, Brazil.
That terrifying moment showed how the scarcity of a medication like hydroxychloroquine can put a lupus patient’s life at risk.
There is still much that needs to be done for lupus patients in Latin America, from speeding up the diagnosis processes, to guaranteeing treatment, to breaking down stigma about ethnicity or the disease itself, to making it possible for them to remain in a labor market that is more inclined to employ men and reject sick women.
What these patients are looking for is not the cold look that Saionara received at a health center in Brazil, but understanding.
"We don't just need medicine, we need conversation," Saionara concludes.
No two cases of lupus are exactly alike. Symptoms may be sudden or develop slowly, may be mild or severe, and may be temporary or permanent.
The most common signs and symptoms include:
Lupus is characterized by organ inflammation. This can affect:
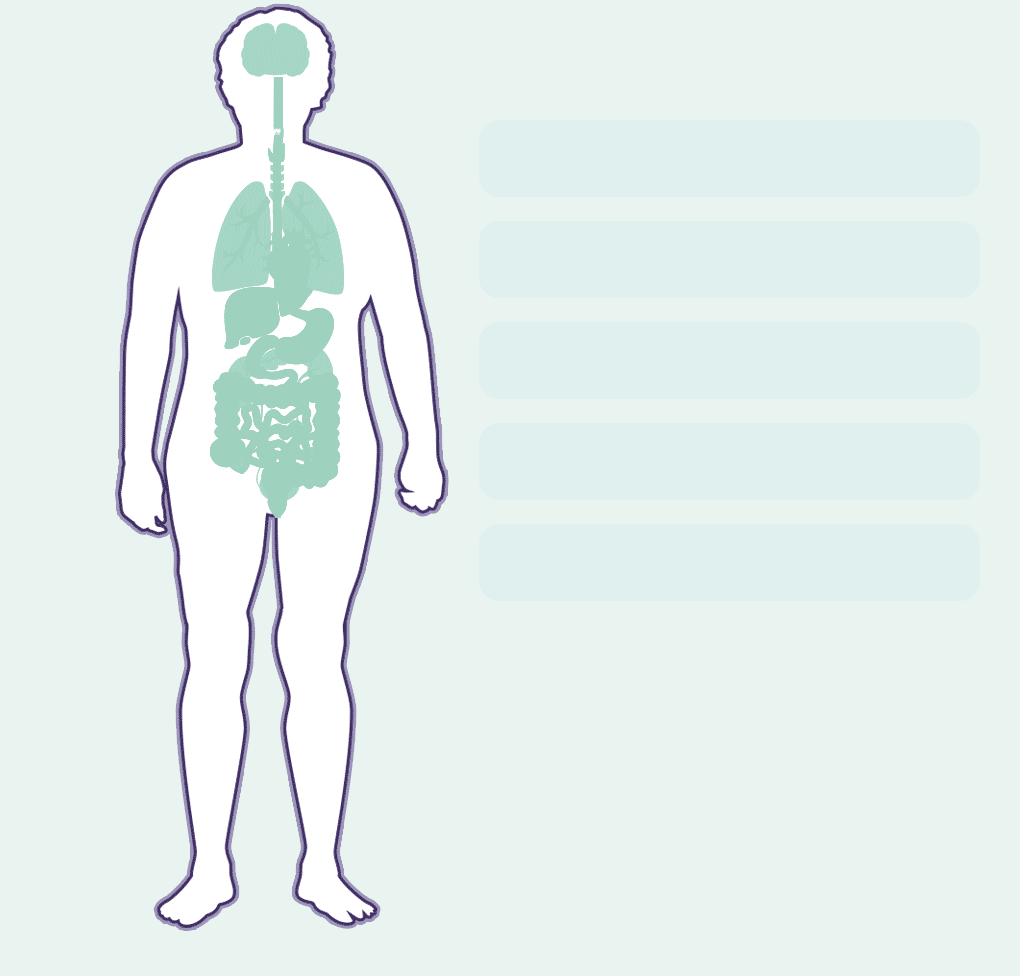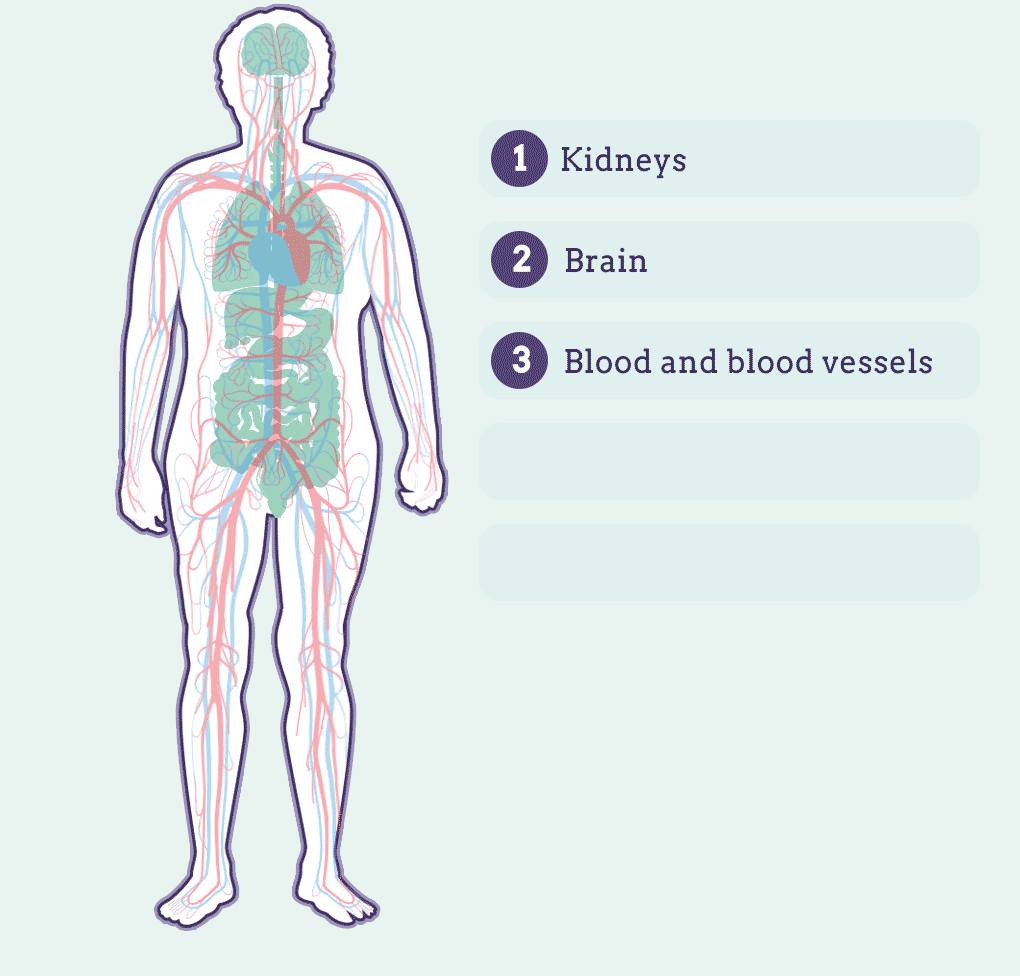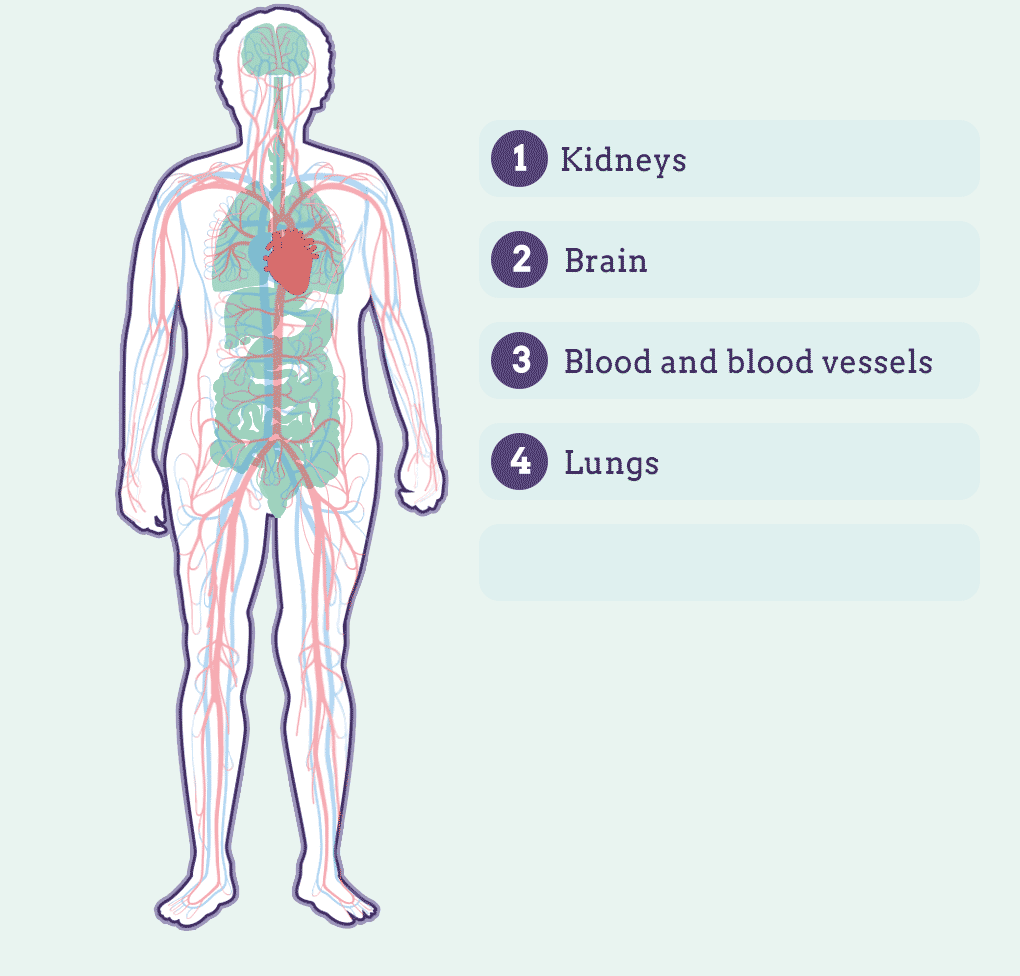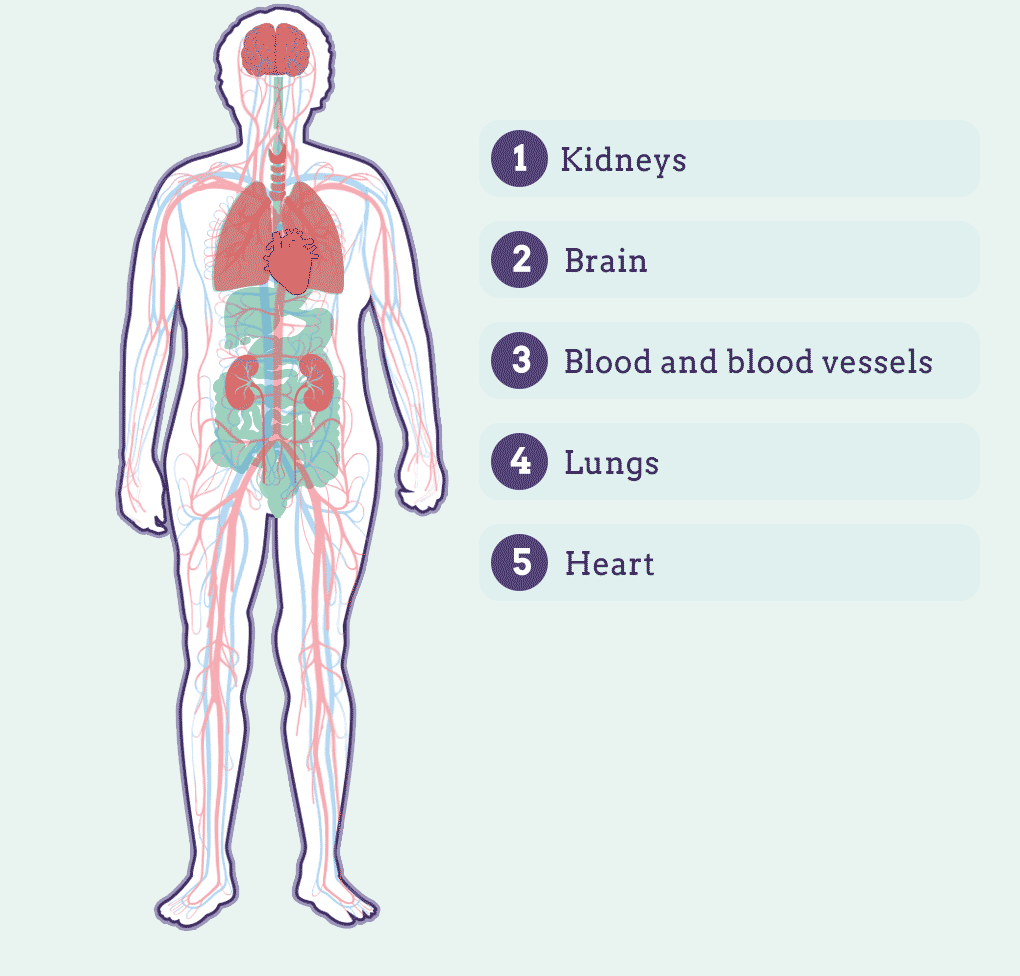
Although there are important scientific advances, there is no specific diagnosis but a series of tests that are applied to determine the patient's symptoms. In addition, symptoms may differ greatly from person to person.
Patients may undergo laboratory analyses such as blood and urine tests that comprise:
Imaging tests may also be applied if lupus is suspected to be affecting the lungs or heart:
FB: facebook.com/lobalupicosorganizadosdabahia/
Phone: +55 71 9 9211-5477
Web: lupus.org.br/site/
FB: facebook.com/superandoolupus
IG: @superandolupus
Phone: +55 11 5574-6438
E-mail: sac@superando.org.br
CNPJ: 04.294.020/0001-73
Phone: +55 21 98782-3254 / +55 21 96763-8237
E-mail: apalurj@bol.com.br
FB: facebook.com/Apalurj
Phone: +55 51 99665-1271 / +55 51 99840-1931
E-mail: lupusvsinos@terra.com.br / alureusocialsl@gmail.com
FB: facebook.com/ALUREU
E-mail: garce.ceara@gmail.com
Phone: +55 85 32412428
Web: garce.org.br/
FB: facebook.com/garcegrupo/
IG: instagram.com/grupogarce
Web: reumatologia.org.br/
FB: facebook.com/sbreumatologia/
Phone: + 55 11 3289-7165
Facebook Groups:
FB: Lupus ayuda Colombia
FB: Lupus Eritematoso Sistémico
FB: Viviendo con Lupus
TW: @GLupusColombia
IG: @grupolupuscolombia
FB: GrupoLupusColombia
IG: @Fundaciongales
TW: @FundacionGales
FB: Fundación Gales - Apoyo Paciente con Lupus
Email: gales.medellin@gmail.com
Phone: 3002656948 | 3015874637
IG: @funluca
FB: Fundacion De Lupus del Caribe
Email: info@funluca.org.co
Phone: 3045454720
fundacionalejandranarvaez.org/
IG: @fundacionalejandranarvaez
TW: @Fundalejanarvae
FB: Fundación Alejandra Narvaez
Email: liliana@fundacionalejandranarvaez.org
Phone: 312 8313187
fundacionlupuscol.wixsite.com IG: @fulucol
FB: Fundación Lupus Colombia Fulucol
Email: fulucol2007@gmail.com
Phone: 312 3595656
FB: facebook.com/appleaslupus/
Email: appleaslupus@gmail.com
Web: web.socreuma.org.pe/
Número de contacto: (+511) 446-1323
Email: socreuma@yahoo.es
Web: somospacientes.com/apelupus/
FB: https://es-la.facebook.com/apelupus.org/
Phone: (01) 2710003
Email: apelupus@apelupus.org
Web: asociacionlupusper.wixsite.com/lupusperuoficial
Phone: 983 589 671
Email: asociacionlupusperu@gmail.com
FB: facebook.com/APPVASOCIACION/
IG: @appv_asoc
Phone: 998 499 428
Web: medicinainterna.net.pe/
Phone: (511) 445-1954
Email: administracion@medicinainterna.org.pe